Author: Sylvia Marinova, PhD student in the Genomic Stability Laboratory at BAS
Photo by Sharon McCutcheon on Unsplash
Type 1 diabetes mellitus, also known by the outdated names insulin-dependent or childhood diabetes, is due to the inability of the pancreas to produce enough of the hormone insulin. Type 1 is the main form of diabetes, which usually occurs in childhood or adolescent age (very rarely in the elderly) and is due from 5% to 10% [ref. 1] of all cases of diabetes mellitus.
Basic information and causes of occurrence
In type 1 diabetes, the pancreas produces very little or no amount of the hormone insulin. It is necessary for the body in order for the main cell fuel coming from food (glucose) to enter from the blood into the cells where it is used for energy.
When there is no insulin, then glucose remains in the blood. This can lead to very high blood sugar and to a state of diabetic ketoacidosis, which is life-threatening (explained below).
Type 1 diabetes is an autoimmune disease, which means that our immune system by mistake attacks the body's own cells. In this case, these are special cells in the pancreas called beta cells, which are responsible for the production of the hormone insulin. This process begins months or years before the first symptoms of the disease are present. With the appearance of a clinical picture, a large part of these cells are already destroyed, sometimes up to 90% of them.
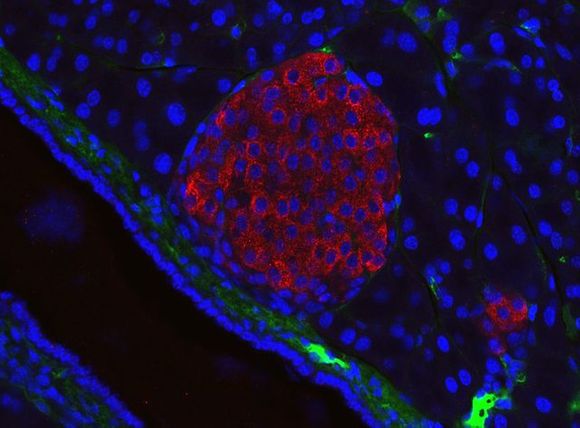
Interesting is the fact that the above-described autoimmune condition is responsible for over 95% of cases of type 1 diabetes. However, in a small proportion of people, the cause of its development is not due to hypersensitivity of the immune system. In these cases, it is not well understood what destroys the beta cells of the pancreas, and then it is said that diabetes is idiopathic [ref. 2] (unknown origin) and is classified as 1b subtype.
Risk factors
Risk factors for type 1 diabetes are not as well studiedas those for type 2 diabetes. However, it is known that defects in the gene system of human leukocyte antigen (HLA) play a significant role and some people are genetically predisposed. This does not mean that they will necessarily develop the disease, but they are more likely to do so.
However, studies with identical twins (individuals with almost the same genome) show that the development of the disease does not always coincide. In other words, this fact suggests that there are other factors, other than heredity, that affect the manifestation of type 1 diabetes. These are most likely environmental factors [ref. 3]. The disease is associated, for example, with some viral infections caused by eneroviruses [ref. 4].
Other risk factors include ethnic ity, obesity and high birth weight.
Genetic causes of type 1 diabetes
The causes of type 1 diabetes are unknown, although several risk factors have been identified. The risk of developing type 1 diabetes is increased by some variants of the genes HLA-DQA1, HLA-DQB1 and HLA-DRB1.
The genes HLA-DQA1, HLA-DQB1 and HLA-DRB1 belong to a family of genes called the Human Leukocyte Antigen Complex (HLA). The HLA complex helps the immune system distinguish the body's own proteins from those produced by foreign invaders such as viruses and bacteria.
Usually type 1 diabetes is considered an autoimmune disease. Autoimmune disorders occur when the immune system attacks the body's own tissues and organs. For unknown reasons in people with type 1 diabetes, the immune system damages beta cells in thepancreas that produce insulin. Damage to these cells disrupts insulin production and leads to the signs and symptoms of type 1 diabetes. [ref. 7]
How to diagnose
Diagnosis of type 1 and 2 diabetes mellitus is usually not complicated. It is a combination of the patient's age, test symptoms and blood tests.
There are three main types of blood tests:
-
Fasting plasma glucose - this test measures the amount of glucose in the fasting blood. To do the examination, it is necessary not to take liquids (the exception makes water) and food at least 8 hours in advance.
-
Glucose-tolerant test - the goal is to assess the body's ability to process glucose. Check the blood sugar level 2 hours after drinking 75 grams of glucose.
-
Glycosylated hemoglobin (HbA1c) - glucose in the blood can be "hooked" to hemoglobin in red blood cells that live between 90 and 120 days. The so-called "no-fly zone" is obtained. glycosylated hemoglobin and it evaluates the average amount of glucose in the blood in the last three months.
After being diagnosed with diabetes mellitus, further tests can be done to distinguish the type.
Photo by National Cancer Institute on Unsplash
Before insulin can be used by the body, it is secreted as proinsulin. This predecessor should be cut in a certain place, thereby receiving two products – active insulin and C-peptide. C-peptide levels can indicate whether the body produces insulin, thereby affecting the state of pancreatic beta cells. In patients with type 1 diabetes, these levels are very low or zero. In patients with type 2 diabetes, levels can vary and even be high, since then there is insulin resistance and insulin production is not always impaired.
Another study that can be done is a blood test to determine the presence of autoantibodies to the beta cells of the pancreas, which testify to processes of their self-de-disruption and therefore speaks of type 1 diabetes.
Symptoms and complications
Patients with type 1 diabetes experience symptomsthat are associated with hyperglycemia (increased blood sugar), which leads to a violation of the balance of fluids and electrolytes in the body. As a result, they appear:
-
polyphagia - a catabolic condition in which glaciers begin to break down fats and proteins due to glucose deficiency. The result of it is weight loss and constant hunger;
-
glucoseuria - the presence of glucose in the urine;
-
polyuria - frequent urination;
-
polydipsia - as a result of dehydration, patients feel increased thirst;
-
blurred vision;
Disorders in the body can be limited by proper and timely treatment that normalizes glucose levels in the blood. If this is not done, then serious complications may arise. One of the most dangerous is diabetic ketoacidosis - ketone bodies accumulate in the blood, and this leads to its acidification. The condition can be life-threatening.
Others are: diabetic retinopathy (damage to the eye stumps and decrease or loss of vision), neuropathy (damage to nerve fibers), nephropathy (kidney disease), diseases of the cardiovascular system, etc.
Treatment
Type 1 diabetes mellitus is a chronic diseasethat lasts a lifetime. Treatment aims to keep the blood sugar level as close to normal as possible to avoid the severe complications it can cause. This requires daily insulin therapy, as well as an appropriate diet combined with regular exercise.
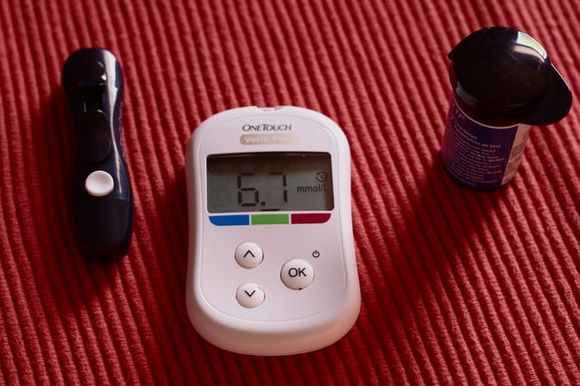
Patients should regulate very well both food intake and the right dose of insulin. Therefore, it is necessary to regularly measure blood sugar through special glucomers, which work with small amounts of blood and report the results very quickly. According to these results, the dosage of insulin is determined with the help of the attending physician.
Some patients use regular syringes to inject insulin ,but other gadgets such as insulin pens already exist. They provide greater convenience and more precise dose measurement. There are also the so-called " some ofthem even have a built-in sensor that detects blood sugar and thus performs strict controlat its level.
It is very important to prevent not only too high blood sugar levels (hyperglycemia), for which it is explained above, but also too low (hypoglycemia). Hypoglycemia is a condition that occurs very quickly as a result of an excess dose of insulin, insufficient food intake or too intense exercise. It is potentially dangerous and should be treated immediately. You may recognize it by symptoms such as dizziness, headache, tremor, weakness, blurred vision, etc.
In milder cases, the intake of a sweetened drink or food is sufficient, but in the more severe cases, intravenous glucose transfusion or injection of glucagon (a hormone that increases blood sugar)may berequired.
Read more about diabetes here:
